- Details
-
Published on 26 January 2018
Alzheimer’s disease, a severely debilitating and ultimately fatal brain disorder, affects millions worldwide. To date, clinical efforts to find a cure or adequate treatment have met with dispiriting failure.
The disease is now on an ominous course of expansion, due in part to an aging population, and is poised to become a global health emergency. The enigmatic ailment—first described over 100 years ago—remains the only leading killer without effective treatment, prevention or cure.
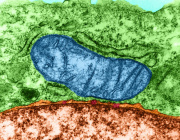
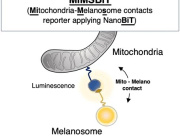
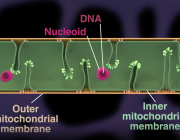
In a new study, researchers at the ASU-Banner Neurodegenerative Disease Research Center examine the effects of the disease on the functioning of mitochondria—structures performing a variety of essential tasks, including supplying cells with energy.
The new research reveals that a highly toxic form of beta amyloid protein— known as oligomeric a-beta (OAβ)—disrupts the normal functioning of mitochondria. The result is a fateful cascade of events that appears early in the development of Alzheimer’s disease—decades before the onset of clinical symptoms.
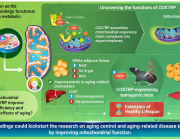
The most promising finding in the new study is that human neuronal cells can be protected from OAβ-induced deterioration of their mitochondria when they are pre-treated with a custom-designed compound, suggesting an exciting avenue for future drug targeting.
"Mitochondria are the major source of energy in brain cells and deficiencies in energy metabolism have been shown to be one of the earliest events in Alzheimer’s disease pathobiology. This study reinforces the toxicity of oligomeric amyloid beta on neuronal mitochondria and stresses the importance for protective compounds to protect the mitochondria from oligomeric amyloid beta toxicity," said Diego Mastroeni, a lead author of the new study.
The research findings appear in "Oligomeric Amyloid Beta Preferentially Targets Neuronal and Not Glial Mitochondrial Encoded mRNAs," made available online by Alzheimer's & Dementia: The Journal of the Alzheimer's Association as an article in press corrected proof.
Mind out of step
Alzheimer's disease, a disorder characterized by severe memory loss, is the most common form of dementia. Most AD cases occur sporadically, with advancing age posing the greatest risk for the disease. Inheritance of certain disease-related genes can also enhance an individual’s susceptibility, though familial AD represents the minority of AD cases.
Two pathological hallmarks are observed in AD brains at autopsy: intracellular neurofibrillary tangles and extracellular senile plaques, which tend to occur in the neocortex, hippocampus, and other subcortical regions crucial for cognitive function. These observations have led to a dominant theory of Alzheimer’s causality, known as the amyloid hypothesis.
The theory points to accumulations of the sticky protein substance amyloid beta as the critical factor initiating the chain of events leading to development of Alzheimer’s disease. While the amyloid hypothesis continues to exert a considerable hold on the field, an increasing consensus among researchers is moving away from the idea of amyloid beta accumulation as the primary event that sets the disease in motion. The new study focuses on mitochondria, which are currently under intense investigation for their early role in AD pathology.
Cells under assault
Alzheimer’s appears to selectively target neurons for destruction and those found in the hippocampus—an area of the brain associated with memory—appear to be particularly vulnerable.
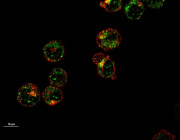
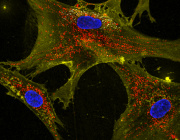
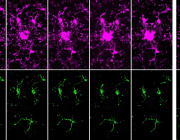
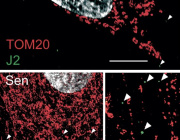
In the new study, cells known as pyramidal neurons, extracted from the hippocampus of patients who died of Alzheimer’s, display a marked reduction in the expression of a suite mitochondrial genes, pointing to their degradation by OAβ. The reduction of mitochondrial gene expression was also seen when cells belonging to a human neuroblastoma cell line were exposed to OAβ.
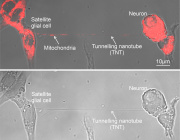
The authors stress that not all types of nervous system cells are implicated in the mitochondrial dysfunction brought on by exposure to OAβ. Hippocampal astrocyte and microglia cells taken from the same AD-afflicted brains did not display reduced mitochondrial function. (Astrocytes and microglia perform supportive functions in the nervous system, including the supply of nutrients, maintenance of chemical balance and cerebral repair following injury.)
Amyloid theory and its discontents
One problem with the amyloid theory of Alzheimer’s disease is its inconsistency. Researchers have reported that some elderly patients, bearing heavy burdens of amyloid plaque in their brains, lack any measurable cognitive deficit, while other patients showing little to no amyloid buildup nevertheless display severe Alzheimer’s-like dementia.
Most damning, a raft of amyloid targeting drugs developed to treat Alzheimer’s have failed to provide any benefit to patients in clinical trials or arrest the inexorable cognitive decline brought on by the disease. It is increasingly apparent that plaques and tangles are late-comers in the devastating sequence of events culminating in Alzheimer’s dementia.
These facts have led researchers to seek other processes occurring at the earliest stages, which may kick the disease into gear. One of the most promising avenues of new research is the mitochondrial cascade hypothesis, which places these energy-delivering powerhouses of the cell at the center of the action.
The hypothesis suggests that mitochondrial function, which declines as a natural feature of aging, may be further impaired in the presence of amyloid beta, in particular, OAb, which is formed from the successive buildup of individual units of Ab. (A million or more individual Ab units may be present in the amyloid plaques that are, along with neurofibrillary tangles, central hallmarks of the disease.) The fact that severe metabolic deficit appears as a prominent feature of AD further implicates energy-delivering mitochondria as likely culprits in the early disease process.
Energy hog
Although the human brain represents only 2 percent of the body’s weight, it accounts for a full 20 percent of the body’s total oxygen consumption. This energy requirement is largely driven by the needs of the brain’s forest of neurons, which require prodigious amounts of energy for their electrochemical signaling. The brain’s intense thirst for energy is continuous; even brief periods of oxygen or glucose deprivation result in neuronal death.
Brain cells fulfil most of their energy needs thanks to the power plants residing in the cell’s cytoplasm—the mitochondria, which supply this energy in the form of ATP. In addition to serving as subcellular organelles essential for generating the energy powering normal cell function, mitochondria also monitor cellular health, and—when necessary—initiate programmed cell death or apoptosis.
Mitochondria however are vulnerable to various forms of decline and degradation. One of the major factors leading to their disruption is a process known as oxidative stress. This results from a disturbance in the balance between the production of reactive oxygen species, known as free radicals, and a cell’s antioxidant defenses.
When anti-oxidant mechanisms can no longer keep pace with the production of reactive oxygen species, mitochondrial gene expression becomes impaired. Oxidative damage is known to occur long before Aβ plaque formation, pointing to mitochondrial dysfunction and oxidative stress in AD as very early players in the disease process.
Lines of evidence
In the new study, researchers compared hippocampal neurons, astrocytes and microglia from AD brains. They used laser capture microdissection, a technique allowing the identification and isolation of each particular cell type, yielding a much more accurate picture of the alterations imposed on specific cell types by the disease. (Traditional methods use brain tissue homogenates containing a mixture of cell types, thereby erasing cell-specific data.)
In complimentary experiments, the group used human neuroblastoma cells exposed to OAβ. Compared with AD neurons, the neuroblastoma cells showed a similar reduction in the expression of specific mitochondrial-encoded genes—strong circumstantial support for OAβ’s injurious effects on mitochondria.
The overlapping effects on gene expression clearly seen in both the AD and OAβ-treated neuroblastoma cells point to OAβ’s selective assault on the nervous system’s energy supply, opening the door for targeted therapy.
In subsequent experiments, human cells were pre-treated in the lab with an analog of CoQ10, (a structural compound capable of boosting ATP production and limiting oxidative stress), prior to exposure to OAβ. The compound, which was designed by study co-author and Biodesign researcher Sidney Hecht, acted to protect cells from the degradation normally caused to mitochondrial function from OAβ, offering renewed hope for effective treatment.
The study further establishes mitochondrial deficit caused by exposure to OAβ as a highly promising avenue for further research in the ongoing battle against this devastating illness.
News credit: richard harth
News source: www.biodesign.asu.edu