Two Blood Markers of Schizophrenia Identified
- Details
- Published on 20 December 2021
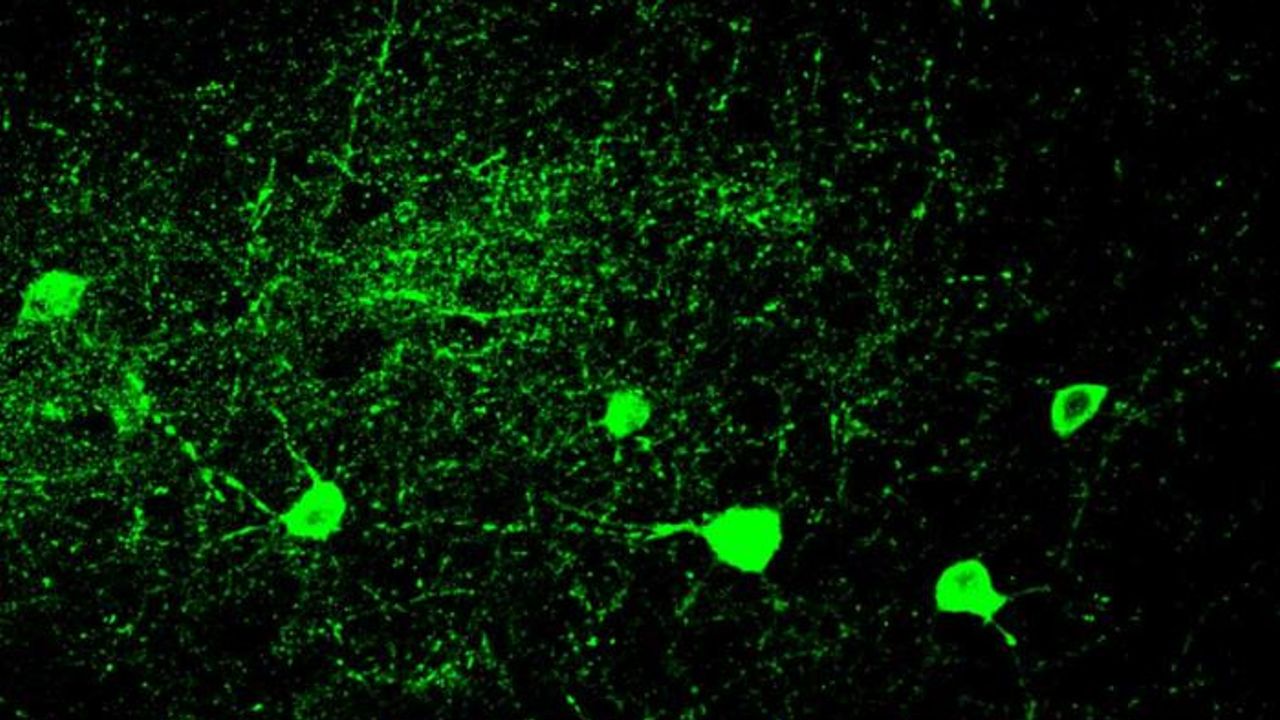
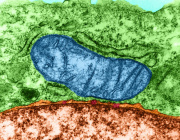
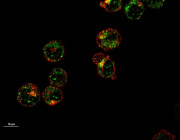
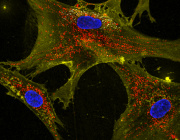
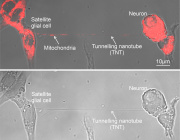
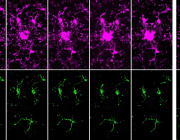
Mouse parvalbumin neurons. Credit: @UNIL/CHUV Inès Khadimallah
This phenomenal research by Synapsy brings us closer to diagnosing Schizophrenia by blood, and treating it.
A research team from Synapsy has shown that the severity of the clinical symptoms of schizophrenia is strongly linked to blood biomarkers related to the deregulation of neuronal mitochondria.
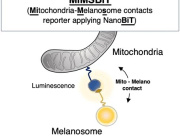
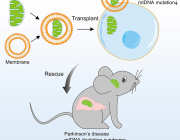
A study conducted at the Centre for Psychiatric Neuroscience of the Lausanne University (UNIL) and the Lausanne University Hospital (CHUV), and supported by the National Centre of Competences in Research Synapsy (Synapsy), has shown, in an animal model, that the cellular mechanism for recycling mitochondria is deficient in parvalbumin neurons.
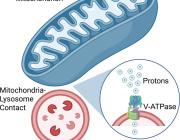
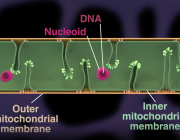
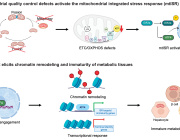
Mitochondria are generally able to eliminate their damaged parts by splitting, using a mechanism called mitophagy. This process involves a series of molecules whose production is controlled by miR137, a microRNA that plays a key role in their regulation. Inès Khadimallah, in collaboration with her colleagues, succeeded in demonstrating that the level of miR-137 was very high in the model, as was oxidative stress. In parallel, an element of cellular respiration expressed specifically by parvalbumin neurons, the COX6A2 molecule is decreased. "In other words, the mitochondria of parvalbumin neurons are dysfunctional following the increase in oxidative stress, and it can be shown through analyzing the levels of miR-137 and COX6A2 in the blood".
In their attempts to intervene directly on the free radicals produced by mitochondria, the neuroscientists showed, in the animal model, that the alterations of these two molecules, miR137 and COX6A2, can be completely corrected by an antioxidant compound that specifically targets mitochondria, called MitoQ.
Keep on track with us and stay updated with all the latest research!